Chronic Constipation: The Silent Epidemic

Whether it’s dehydration, not getting your 5 a day, painkillers, stress or even holding it all in for days at Glastonbury – there are many causes of constipation. Despite this, it’s not exactly water cooler chat at work and too many of us suffer in silence. Luckily, our amazing gastroenterologist Dr Reshma Rakshit is on hand to give us the low-down on constipation in her characteristic expert and down-to-earth style…
“I am passionate about the workings of the digestive tract. That’s a good thing, given that I’m a gastroenterologist!
One of the common problems I deal with in clinic is constipation. Yes, you’ve read it right. It is a common, but sometimes poorly treated condition. Often, the problem is linked to the reluctance or embarrassment associated with discussing details of bowel movements. Sometimes, healthcare providers can trivialise it as a minor ailment, though, it wreaks havoc on many people’s lives.”
A recent study conducted in England revealed that the general public was not entirely sure of what constipation meant, and their thoughts differed significantly from health care professionals. Most doctors seem to relate constipation with reduced bowel frequency but most of the public relate it to straining or difficulty in the passage of stools. One way to address this would be through education, by raising the profile of constipation and its treatment options.
Patients suffer in silence, with or without medication. Another study showed that up to 50-70% of people were dissatisfied with the results of using laxatives for constipation.
The function of your bowel
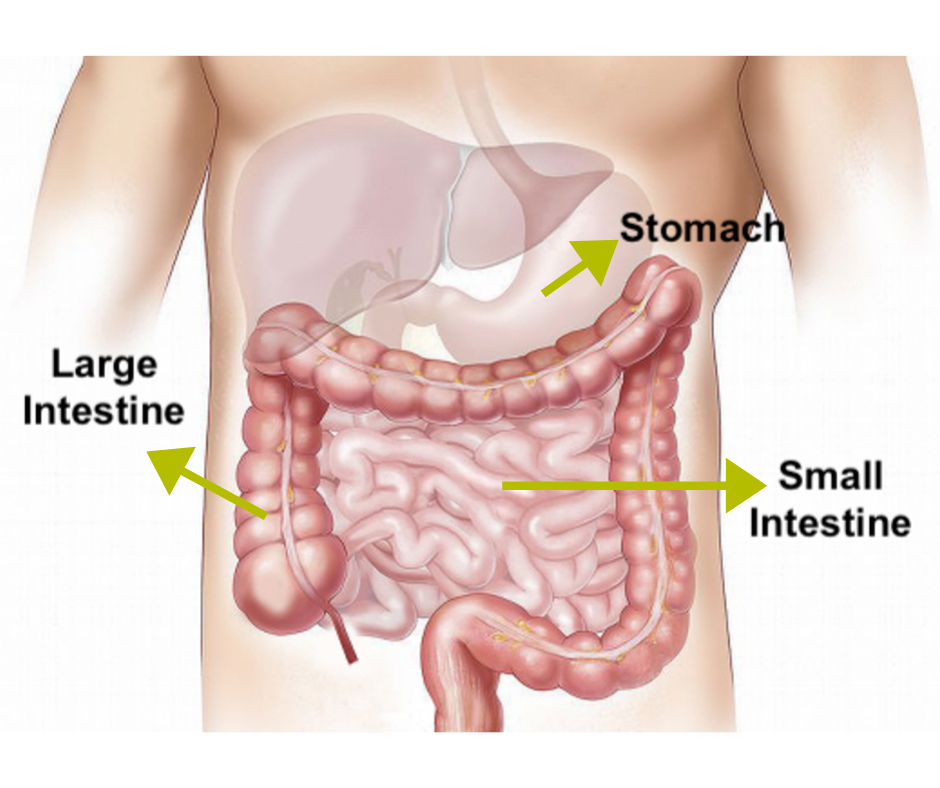
The digestive tract helps to digest the food and drink that we consume. Liquid waste of digestion flows from the small intestine (small bowel) to the large intestine (also known as large bowel or colon).
The function of the colon is 3 fold. Firstly, it absorbs the water from the liquid waste to change it into solid waste. Secondly, the involuntary muscles of the colon, move the waste along. Thirdly, the lower end of the colon, which is called the rectum, stores the solid waste, until it is the right time for evacuation. The later function is dependant on social situations, for example, the right time for bowel clearance (in the morning or after a meal), relationship with the mind (stress and anxiety can cause disturbance of this function) and the correct pelvic floor muscle mechanism, amongst a myriad of other complex known and unknown factors.
What is constipation?
Constipation is simplistically defined as difficulty in bowel movements. It can be acute (sudden in onset) or chronic which means the symptoms have lasted for more than 6 months. The symptoms include one or more of the following:
- Reduced frequency of bowel movements
- Straining during passage of stools
- Passing hard rabbit pellet-like motions
- Dissatisfaction after a bowel movement – feeling of incomplete emptying
- Feeling of a lump in the lower end of the bowel
- Using fingers to help push the stools out from the rectum
- Bleeding from the bottom end
- Bloating of the abdomen, nausea and abdominal cramps.
Worrying symptoms to look out for, especially if there is a sudden change, including bleeding from the back passage, weight loss, tummy pain, a lump in the tummy, severe fatigue or tiredness or anaemia. In such cases, further assessments would be prudent to exclude serious medical conditions.
What causes constipation?
Constipation is a symptom, not a diagnosis. The cause is not always easy to explain, and in some patients, no cause can be found. However, there are some possible factors, as detailed in the table below.
- Diet: not enough soluble fibre (oats, fruits, vegetables, whole grains).
- Fluid: not drinking enough non-caffeinated fluids.
- Immobility: after, for example, an operation or poor daily activity.
- Increasing age: bowel muscles can become weaker with age and less active lifestyles can lead to constipation.
- Medication: some pills can cause constipation (some pain killers, water tablets, antacids)
- Environmental changes: on holiday or changes in toilet access.
- Medical conditions: some conditions have associated constipation (Irritable bowel syndrome, cancer, Parkinson’s disease, spinal cord damage or stroke)
- In-coordination or weakness of the pelvic floor muscles (after childbirth, menopause)
- Mental health issues, like anxiety or depression, can lead to constipation.
The bowel wall muscles need enough stool bulk (amount) to work on. The fibre helps increase the bulk by holding onto water. So, if you don’t eat enough soluble fibre and fluid, there will not be enough impetus to move the waste along. The longer the stools stay in the bowel, the more water is absorbed and the stools become harder. This, in turn, is harder to shift. Finally, hard stools, maybe too hard for the pelvic floor muscles to overcome This leads to a vicious cycle of chronic constipation. Other factors make an impact, depending on the person-specifics.

Treatments and recommendations
Listening to patients is key: sometimes, that alone can help the situation. I take a detailed dietary, medical and lifestyle history. I look out for worrying signs and symptoms and only a small number of patients need investigations. These can include blood tests, X-rays, camera tests into the bowel (colonoscopy) or CT scan of the bowel (virtual colonoscopy). Further management is individualised.
Diet
Many of my patients get referred to a dietician to optimise their dietary intake of fibre. This can be in the form of introducing dietary fibre, like fruits, vegetables and certain grains. If that doesn’t work, golden linseeds can be beneficial. Alternatively, adding psyllium (natural plant-based fibre supplement) can be bought “over the counter” to help. Enough fluid is essential for these to work. Sometimes, bloating can be an issue and therefore these changes need to be made slowly and monitored.
Lifestyle modification
Lifestyle modification is important including understanding the mechanism of bowel evacuation. It is important to have a bowel evacuation routine or habit. Correct posture, being in a “comfortable “ space for evacuation and avoiding postponing the urge to “go”, are vital. Increasing exercise or daily activity is important too. I have provided a common example in the box below.
- Eat enough soluble fibre
- Drink enough non-caffeinated drinks
- Stay active
- Have a regular routine for bowel movements
- Adopt the correct posture during passage of stools
- Avoid straining
- Avoid ignoring the urge to open your bowels
- Manage stress
In summary, I would like to reassure people that constipation is common and manageable in most patients. You don’t have to suffer in silence. Talking to a doctor or health care professional would help if simple measures do not work. If these do not relieve the symptoms, seek for a specialist opinion as there are new interventions that help relieve the symptoms and allow for a more comfortable bowel pattern and life.
DISCLAIMERS: This is not a substitute for medical advice- please see your GP for a proper consultation. This article deals with adults only.
Medstars Medical Concierge Service
Looking for extra guidance when it comes to your healthcare? Sometimes interpreting medical information and making the best decisions can be daunting and complicated. Our private medical concierge service provides easy access to top UK health experts. We guide our patients with genuine choice and trust, offering a bespoke service for anyone in the world seeking private UK healthcare. Learn more about Medstars Medical Concierge Service. Want to learn more about providing our medical concierge service as an employee benefit? Learn more about Medstars Medical Concierge for Business.

